An advanced form of adoptive cellular immunotherapy that harnesses and enhances the patient’s own immune system to recognize and eliminate malignant cells with high specificity.
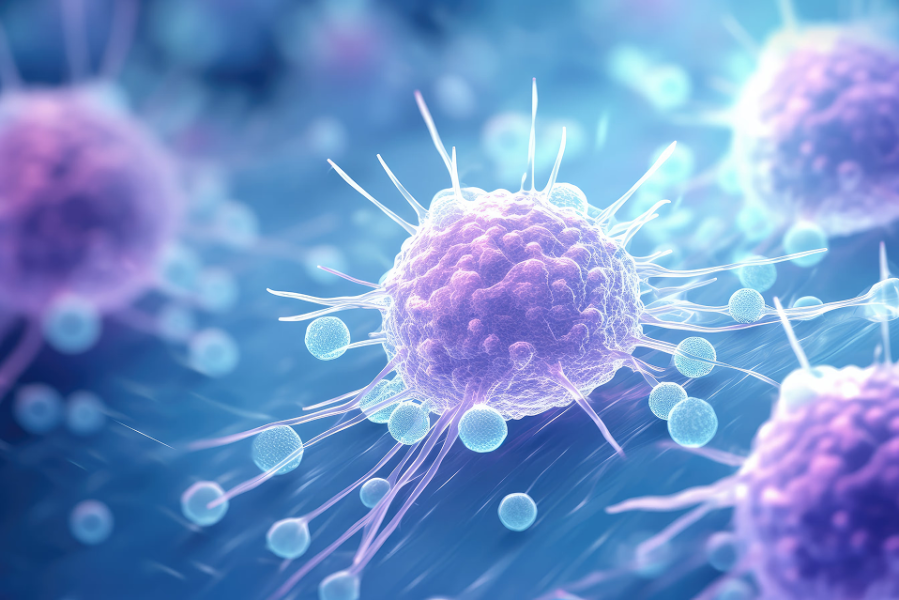
Response In Leukemia
Approved Therapy
Single Infusion

Typically derived from a monoclonal antibody, this extracellular domain allows the T-cell to lock onto specific cancer cell markers.
This structural component anchors the receptor to the T-cell surface, ensuring stability during the attack phase.
Domains such as CD3ζ and costimulatory molecules like CD28 or 4-1BB activate the T-cell to proliferate and destroy the target.
Specifically engineered to target cancer cells while sparing most healthy tissues.
The ability to induce long-lasting remission even in advanced stages.
Modified cells can persist in the body, providing ongoing protection against recurrence.
Effective in treatment-resistant or relapsed cancers where other lines have failed.
High success rates in treating children and young adults.
A leading treatment for this aggressive type of non-Hodgkin lymphoma.


CAR T-cell therapy is an advanced immunotherapy in which a patient’s own T cells are genetically modified to better recognize and attack cancer cells, then reinfused back into the body.
It is primarily used for certain blood cancers, including specific types of leukemia and lymphoma. It is FDA-approved and shows high response rates in eligible patients.
Success varies by cancer type, but in some forms of leukemia, response rates can reach up to 90%.
TIL (Tumor-Infiltrating Lymphocyte) therapy is an immunotherapy approach in which a patient’s own immune cells are harvested, expanded in the laboratory, and reinfused to fight cancer.
No. TIL therapy is currently used more commonly in certain solid tumors, especially metastatic melanoma. Patient suitability is determined on an individual basis.
Its personalized nature and its ability to strengthen the immune system in a targeted way are considered its main advantages.